Have you ever had weeks where you feel like you’re on top of the world—crushing your workouts, acing your projects, and being the life of the party? And other weeks where you feel so drained that just getting off the sofa feels like a marathon?
What if I told you that those energy shifts aren’t random? They’re actually connected to the natural hormonal rhythm of your menstrual cycle. And you can use that rhythm to your advantage.
Welcome to the world of cycle syncing. It sounds fancy, but it’s actually super simple: it’s the practice of aligning your lifestyle (think exercise, work, and even your social life) with the different phases of your menstrual cycle. Instead of fighting against your body’s natural flow, you learn to work with it.
At CrampCare, we believe this is one of the biggest wellness superpowers you can unlock. Let’s get into how you can stop swimming against the current and start riding the wave.
The Four Seasons of Your Cycle
Think of your cycle as having four distinct seasons, each with its own unique hormonal landscape and energy level.
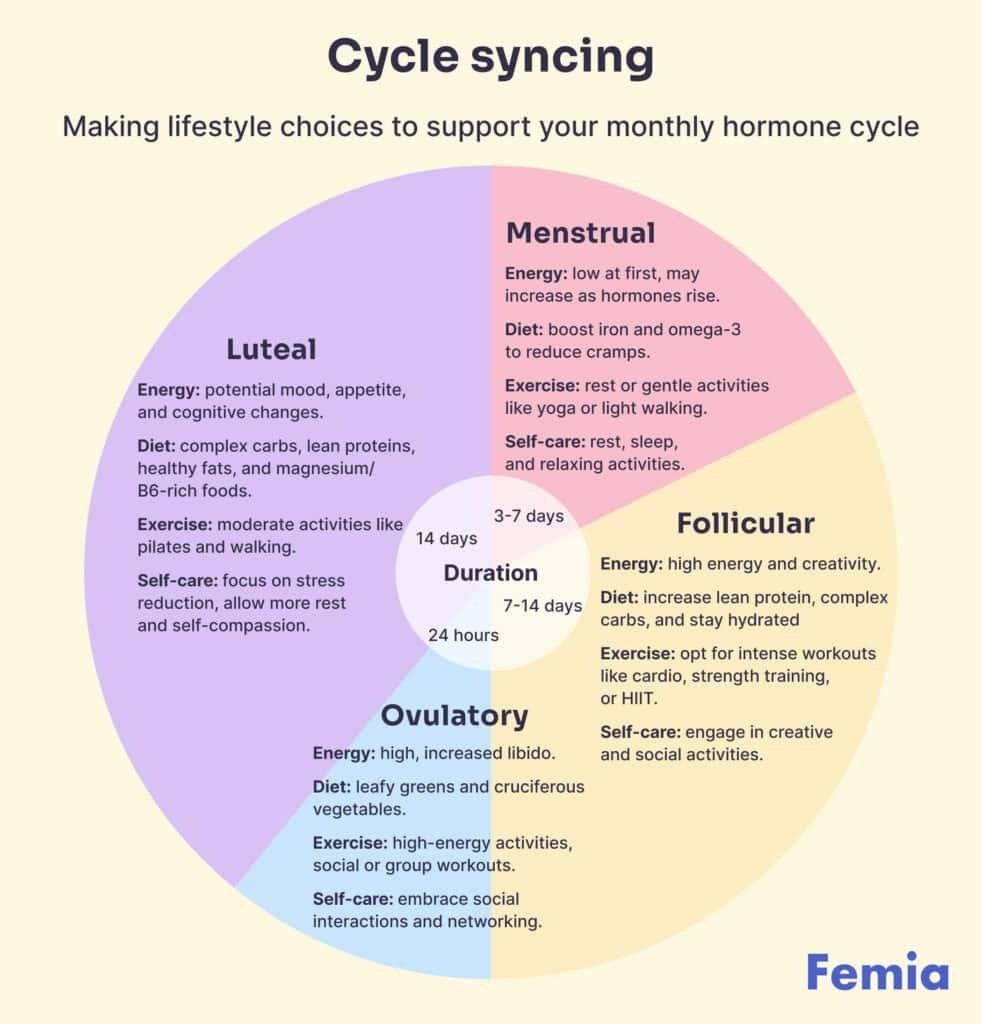
Source: Femia
Phase 1: Menstrual (Your Period – The “Winter” ❄️)
- What’s Happening: Your hormones (estrogen and progesterone) are at their lowest point. Your body is shedding your uterine lining. It’s a time for rest and release.
- Your Vibe: Low energy, intuitive, reflective.
- Sync Your Life: This is your permission slip to slow down.
- Exercise: Think restorative and gentle. Go for a walk, do some gentle stretching, or try a yin yoga class.
- Work: Your two brain hemispheres are most connected now, making it a great time for reflection and evaluation. Review projects, journal, and avoid tight deadlines if you can.
- Social Life: Honor your need for alone time. A cozy night in with a book or a movie is perfect. Say no to big social events if you’re not feeling it.
Phase 2: Follicular (Before Ovulation – The “Spring” 🌱)
- What’s Happening: Estrogen is starting to rise, which boosts your energy, mood, and brainpower. You’re emerging from your winter hibernation.
- Your Vibe: Creative, energetic, open to new things.
- Sync Your Life: Plant the seeds for the month ahead.
- Exercise: Your energy is returning, so you can start to ramp things up. Try cardio, light runs, or a fun dance class.
- Work: This is your brainstorming phase. Start new projects, learn a new skill, and map out your goals.
- Social Life: You’re feeling more social. Plan a fun outing with friends or go on a date.
Phase 3: Ovulatory (Ovulation – The “Summer” ☀️)
- What’s Happening: Estrogen and testosterone are at their peak! This is when you release an egg. You’re at the height of your power.
- Your Vibe: Confident, social, communicative, magnetic.
- Sync Your Life: It’s time to be seen and heard.
- Exercise: Go all out! This is the best time for high-intensity workouts like HIIT, spinning, or heavy lifting. Your body can handle it.
- Work: You’re a communication superstar right now. Schedule important meetings, give that presentation, ask for a raise, or have that difficult conversation. Collaborate with others.
- Social Life: This is your social peak. Host the party, go to the networking event, and connect with people.
Phase 4: Luteal (Before Your Period – The “Autumn” 🍂)
- What’s Happening: Progesterone is rising, and if the egg wasn’t fertilized, both estrogen and progesterone will start to fall, leading to PMS symptoms. Your energy begins to wind down.
- Your Vibe: Detail-oriented, focused, a little introverted.
- Sync Your Life: It’s time to wrap things up and get cozy.
- Exercise: Start to scale back the intensity. Focus on strength training, Pilates, or more moderate cardio. As you get closer to your period, shift back to more gentle movement.
- Work: Your focus shifts inward, making this a great time for detail-oriented tasks. Finish up projects, organize your files, and clear your to-do list.
- Social Life: You might feel more like nesting. Plan a small get-together with close friends or a cozy date night at home.
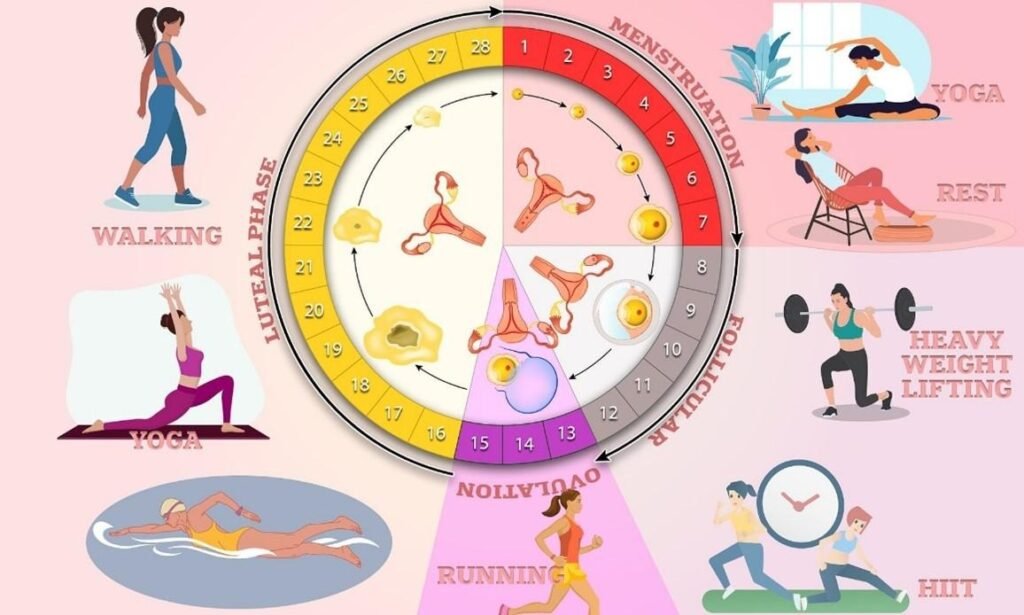
How to Start Cycle Syncing: The First Step is Easy
Feeling overwhelmed? Don’t be. You don’t have to do all of this at once. The most important first step is simply to start tracking your cycle. You can’t sync with a rhythm you don’t understand.
This is where the CrampCare app becomes your best friend. By tracking your period, symptoms, and mood every day, you’ll start to see your own unique patterns emerge. You’ll learn exactly when your personal “spring” begins and when it’s time to prepare for your “autumn.”
Start small. This month, maybe just try to sync your workouts. Next month, focus on your work tasks. It’s not about being perfect; it’s about being in tune with your body.
Working with your body instead of against it is a radical act of self-care. Welcome to the flow.






