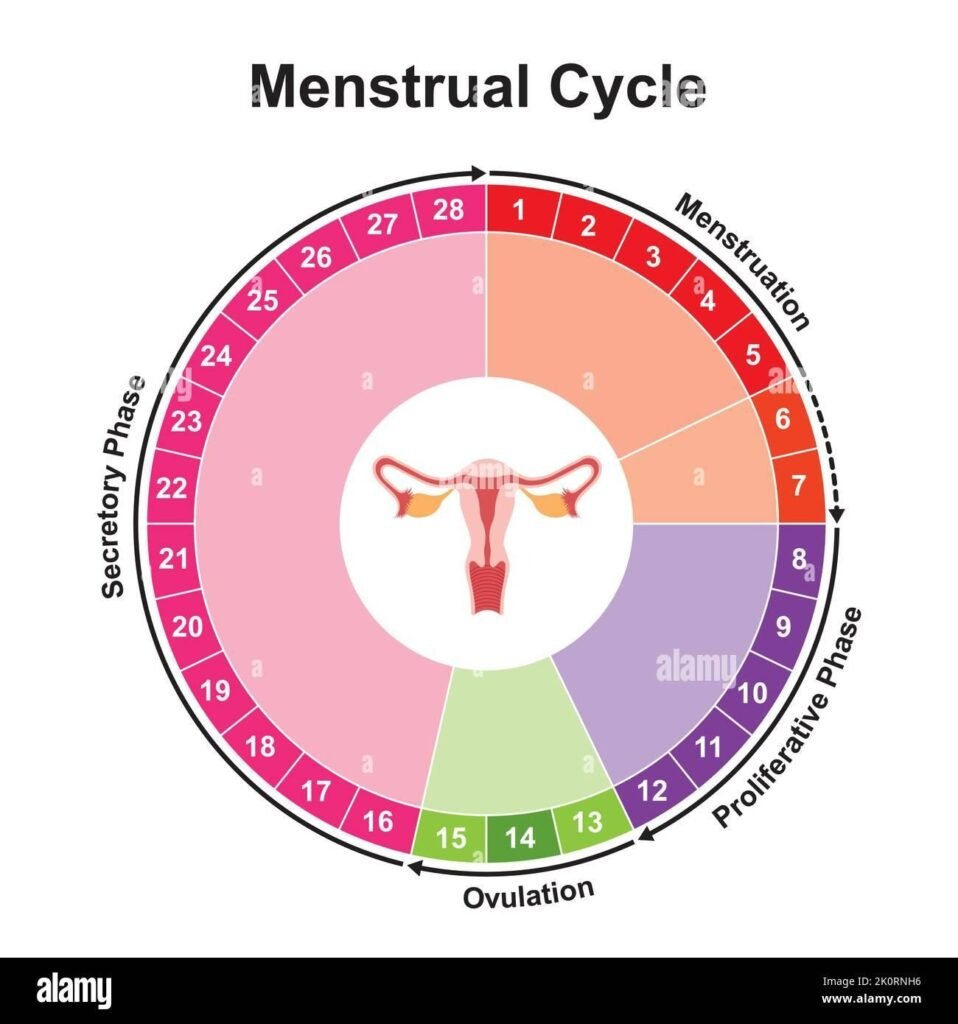
We’re taught to just “deal with” our periods. We learn to push through the pain, manage the bleeding, and accept that our bodies are just going to do their own thing. But what if “dealing with it” means missing out on life? What if your period problems feel like more than just a monthly inconvenience?
It can be really hard to know what’s “normal” and what’s a sign that you should get help. We often downplay our own pain or assume everyone feels the way we do.
At CrampCare, we want you to know one thing: your pain is valid, and you don’t have to suffer in silence. Knowing when to raise your hand and ask for help is a superpower. Let’s go over the key signs that mean it’s time to check in with a doctor.
The “When to Worry” Checklist
Think of this as your guide to listening to your body. If any of these sound familiar, it’s a good reason to make an appointment.
1. Your Pain is Next-Level
We’re not talking about the usual, annoying cramps that a heating pad can fix. We’re talking about pain that stops you in your tracks.
See a doctor if:
- Your period pain is so bad you regularly have to miss school, work, or social events.
- Over-the-counter pain meds like ibuprofen (Advil) or naproxen (Aleve) barely make a dent.
- The pain has been getting worse over time.
- You have significant pain even when you’re not on your period.
This kind of severe pain isn’t something you just have to live with. It could be a sign of a condition like endometriosis or fibroids, and there are treatments that can help. [1]
2. Your Bleeding is Super Heavy
What’s a “heavy” flow? It can be subjective, but there are some clear signs that your bleeding is more than average.
See a doctor if:
- You have to change your pad or tampon every hour for several hours in a row.
- You have to wake up at night to change your protection.
- Your period consistently lasts longer than 7 days.
- You pass blood clots that are bigger than a quarter.
Extremely heavy bleeding (the medical term is menorrhagia) can lead to anemia, which can make you feel tired and weak. It’s also a common sign of underlying issues that a doctor can help you manage. [2]
3. Your Cycle is All Over the Place
As we’ve said before, a perfect 28-day cycle is a myth. But a cycle that’s consistently unpredictable is worth looking into.
See a doctor if:
- Your cycles are always shorter than 21 days or longer than 35 days.
- You go more than 3 months (90 days) without getting a period (and you know you’re not pregnant).
- Your cycle length suddenly changes dramatically and stays that way for a few months.
- You bleed or spot between your periods.
Irregular cycles can sometimes be the first sign of a hormonal imbalance, like with Polycystic Ovary Syndrome (PCOS) or a thyroid condition.
How to Talk to Your Doctor and Be Heard
Okay, so you’ve decided to make an appointment. Awesome! The next step is to prepare so you can have the best possible conversation. Unfortunately, some doctors can be dismissive of period pain, so walking in with clear information is your best strategy.
1. Come with Data: This is your secret weapon. Instead of just saying “my periods are bad,” you can say “For the last four months, I’ve had debilitating pain for the first two days of my period, and I’ve had to miss two days of work each time.” See the difference?
2. Track Everything: This is where an app like CrampCareis a lifesaver. Before your appointment, use it to track:
* The start and end dates of your period.
* Your pain levels each day (a 1-10 scale is great).
* How heavy your flow is (light, medium, heavy).
* Any other symptoms (like clots, bloating, mood swings, or pain with sex).
* What you did to try and manage the pain (meds, heat, etc.) and whether it helped.
3. Have Your Questions Ready:Write down a few key questions you want to ask. For example:
* “Based on my symptoms, could this be more than just normal period pain?”
* “What tests could we do to find out more?”
* “What are my treatment options besides birth control?”
Walking into a doctor’s office with a detailed log from your CrampCare app changes the conversation. It shows you’re serious and gives your doctor concrete evidence to work with. You are the expert on your body; the data just helps you prove it.
Don’t let anyone tell you it’s “just a bad period.” If your cycle is controlling your life, you deserve answers. Take that first step, talk to a doctor, and start your journey to feeling better.
References
[1] American College of Obstetricians and Gynecologists. (2022). Dysmenorrhea: Painful Periods. https://www.acog.org/womens-health/faqs/dysmenorrhea-painful-periods
[2] Centers for Disease Control and Prevention. (2022). Heavy Menstrual Bleeding. https://www.cdc.gov/ncbddd/blooddisorders/women/menorrhagia.html