Making the decision to start a family is a huge, exciting step! It’s a journey filled with hope, daydreams, and a whole lot of love. But it can also come with a lot of questions and a bit of pressure. You might be wondering, “Am I doing everything I can? How can I make this happen?”
Trying to conceive (TTC) can feel like you’re navigating a whole new world, and it’s easy to get overwhelmed by all the advice out there. At CrampCare, we want to walk alongside you on this path, offering clear, supportive, and empowering advice to help you on your journey to parenthood.
Let’s talk about the most effective ways to boost your fertility and increase your chances of seeing that positive test, one gentle step at a time.
1. Timing is Everything: Get to Know Your Fertile Window
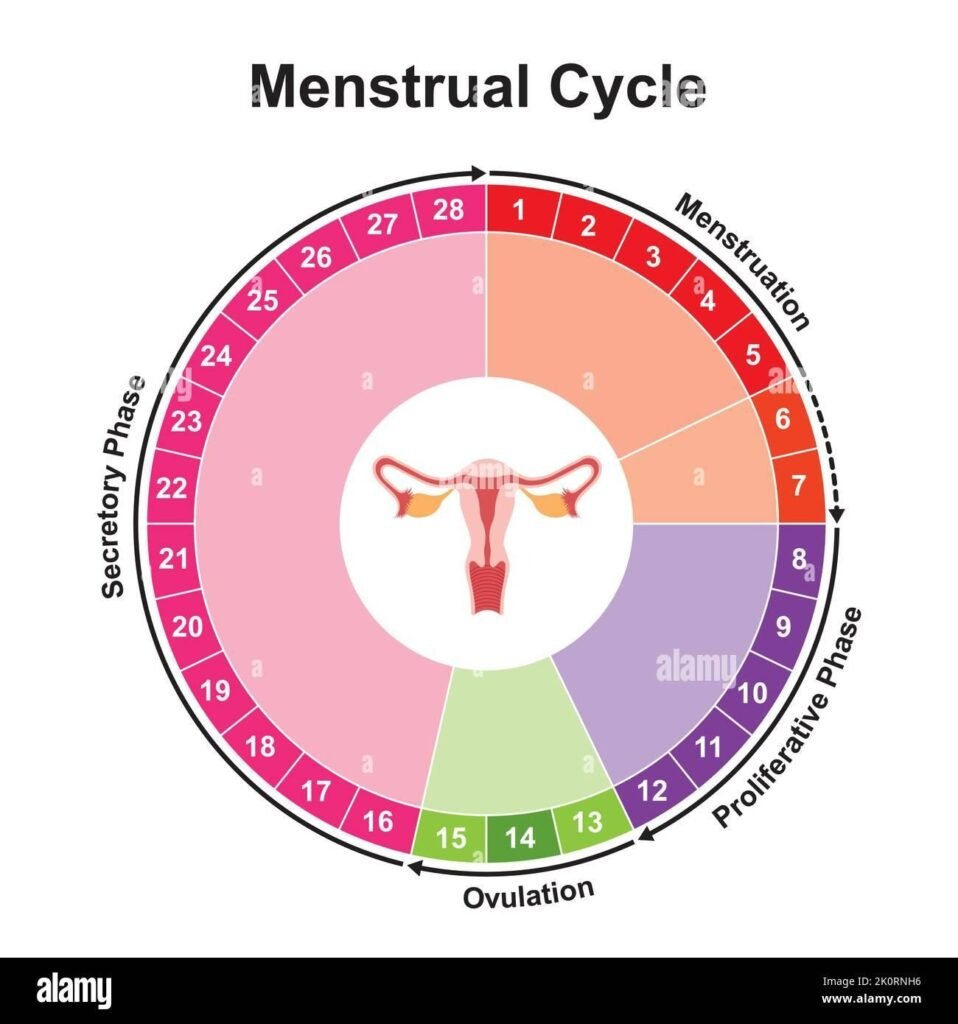
If there’s one “secret” to getting pregnant, this is it. You can only conceive during a very specific time in your cycle known as the fertile window. This window is about 6 days long: the 5 days before you ovulate and the day you ovulate.
Having sex during this window is the single most important thing you can do to increase your chances of getting pregnant. [1]
So, how do you find this magic window? By becoming an expert on your own cycle. You can do this by tracking a few key signs:
- Your Cycle Length: Helps you estimate when ovulation might happen.
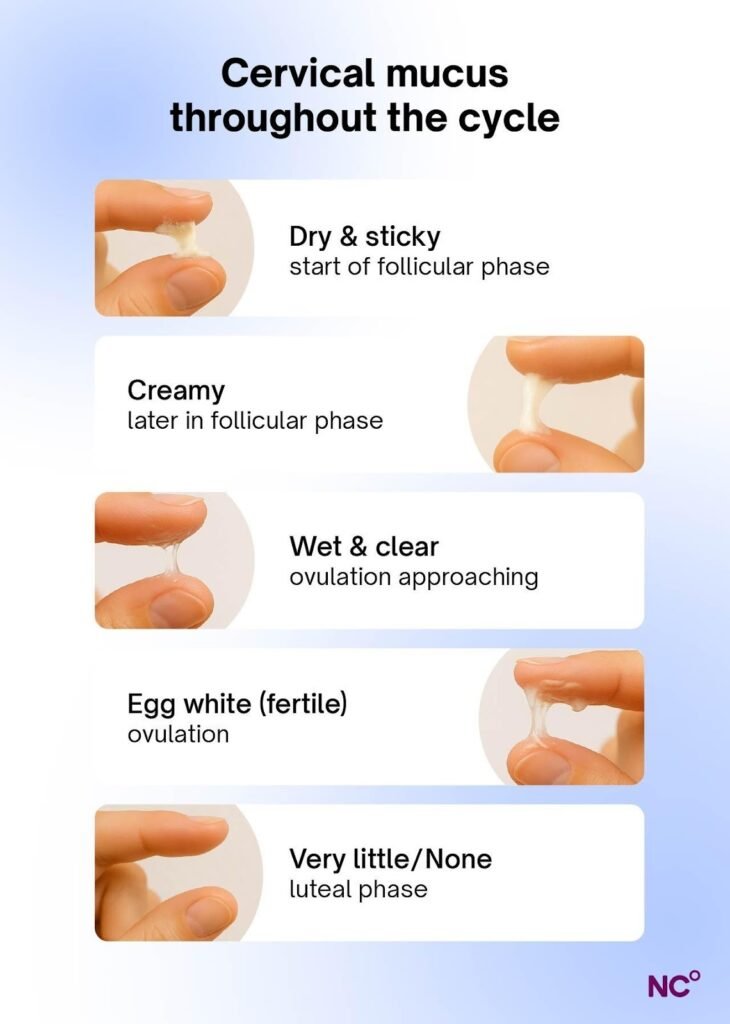
- Your Cervical Mucus: Changes to a clear, stretchy “egg white” consistency when you’re most fertile.
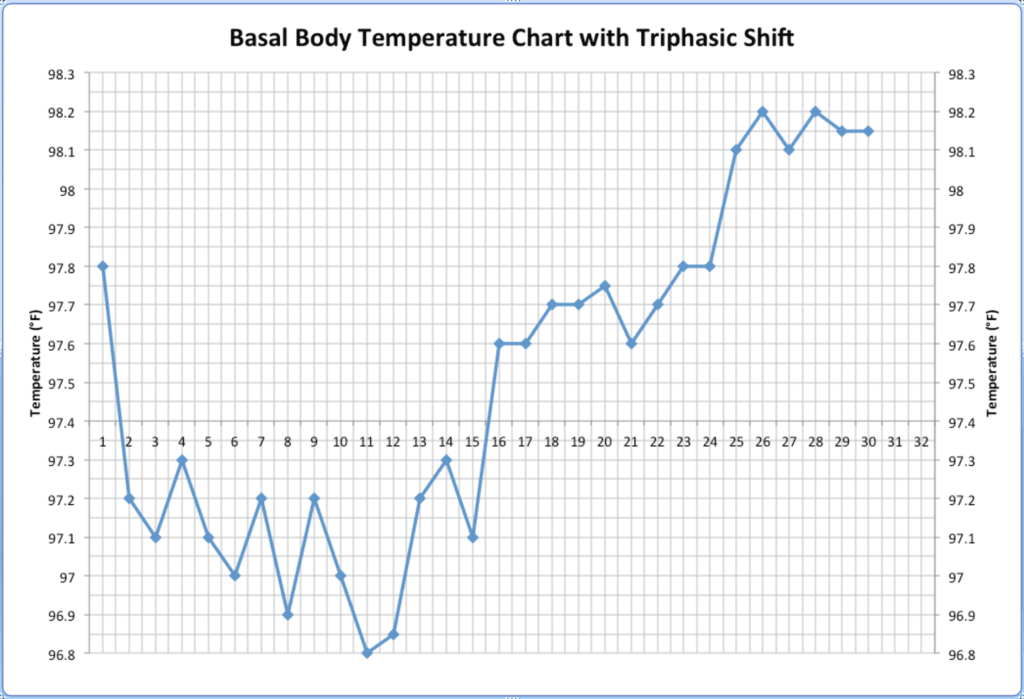
- Your Basal Body Temperature (BBT): Spikes slightly right after ovulation, confirming it happened.
This is where an app like CrampCare becomes your best friend. It takes the guesswork out of tracking and helps you pinpoint your most fertile days with confidence, so you can focus on the fun part!

2. Nourish Your Body: The “Fertility Diet”
Think of your body as a garden you’re preparing for a beautiful new seed. Creating a healthy, nourished environment is key. While there’s no magic food that guarantees pregnancy, a balanced, nutrient-rich diet supports your overall health and hormone function, which is crucial for fertility.
Focus on these Fertility-Friendly Foods:
- Leafy Greens: Spinach, kale, and broccoli are packed with folate, a B vitamin that’s essential for preventing birth defects and supporting reproductive health.
- Healthy Fats: Avocados, nuts, seeds, and olive oil help regulate your hormones.
- Lean Proteins: Think fish, chicken, beans, and lentils.
- Complex Carbs: Brown rice, quinoa, and whole-wheat bread provide sustained energy without spiking your blood sugar.
It’s also wise to limit things that can work against you, like excessive alcohol, smoking, and too much caffeine. [2]
3. Move with Joy: Finding Your Exercise Sweet Spot
Regular, moderate exercise is fantastic for fertility. It helps you maintain a healthy weight, reduces stress, and improves circulation. The key word here is moderate.
This isn’t the time to train for a marathon or push yourself to the absolute limit. Over-exercising can actually stress your body and interfere with ovulation. Instead, focus on movement that feels good and energizes you.
Great options include:
- Brisk walking or hiking
- Gentle yoga or Pilates
- Dancing
- Swimming

Source: LIVE FERTILE
4. Find Your Calm: Why Stress Matters
The TTC journey can be stressful, which is a cruel irony because high levels of stress can mess with the hormones that control ovulation. Finding healthy ways to manage stress is not just good for your mental health—it’s good for your fertility, too.
Try incorporating some of these into your routine:
- Mindfulness or Meditation: Even 5-10 minutes a day can make a difference.
- Deep Breathing: A simple tool you can use anytime, anywhere.
- Journaling: Get your worries out of your head and onto paper.
- Prioritizing Sleep: Aim for 7-9 hours of quality sleep per night.
Be kind to yourself. This journey is a marathon, not a sprint.
When to Get a Little Extra Help
It’s also important to know when it might be time to talk to a professional. The general guidelines are:
- If you are under 35 and have been actively trying for one year.
- If you are over 35 and have been actively trying for six months.
You should also consider seeing a doctor sooner if you have a history of very irregular periods, PCOS, endometriosis, or other known health issues.
A doctor can help you explore your options and create a plan that’s right for you. Remember, seeking help is a sign of strength.
You’ve Got This
Embarking on the path to parenthood is a profound and personal experience. Be patient with your body, celebrate the small victories, and lean on your partner and support system.
Let CrampCare be your trusted companion on this journey, helping you understand your body and feel empowered every step of the way. You are capable, you are strong, and you’ve got this.
References
[1] American Society for Reproductive Medicine. (2021). Fertility and Sterility: Optimizing natural fertility. https://www.fertstert.org/article/S0015-0282(16)62895-9/fulltext
[2] American College of Obstetricians and Gynecologists. (2021). Evaluating Infertility. https://www.acog.org/womens-health/faqs/evaluating-infertility